A once rare allergy to meat is becoming less so and is estimated to affect nearly half a million Americans. Unlike typical allergies triggered by proteins, Alpha-Gal Syndrome (AGS) is linked to a carbohydrate molecule called alpha-gal which is common to mammals. The culprits are mostly Lone Star ticks, predominantly found in the southeastern United States. When these ticks bite, they inject alpha-gal into the bloodstream, allowing the immune system to develop antibodies to the carbohydrate. Thus, the immune system may cause an allergic reaction the next time you eat mammalian meat like beef, pork, or lamb.
What makes AGS particularly tricky is its delayed reaction. Symptoms such as nausea, vomiting, hives, and even anaphylaxis (low blood pressure, trouble breathing) can strike three to six hours after a meal.
The diagnosis relies on detailed patient histories, noting tick bites and meat-related symptoms, and the use of blood tests that detect specific IgE antibodies to alpha-gal.
Living with AGS means making significant lifestyle adjustments. Avoiding mammalian meat and products containing alpha-gal is essential but challenging, given its presence in some medications and processed foods. For those affected, antihistamines can manage mild symptoms, while carrying an epinephrine auto-injector is a lifesaver for severe reactions. Preventing tick bites is equally crucial, involving repellents, protective clothing, and meticulous tick checks after outdoor activities.
Research into AGS is ramping up, with scientists exploring the allergy’s mechanisms and seeking better diagnostic tools and treatments. As tick populations rise and spread, awareness and understanding of AGS are more critical than ever.
For additional information and resources, like the map below, visit the CDC’s website.
FIGURE. Geographic distribution of suspected alpha-gal syndrome cases* per 1 million population per year — United States, 2017–2022
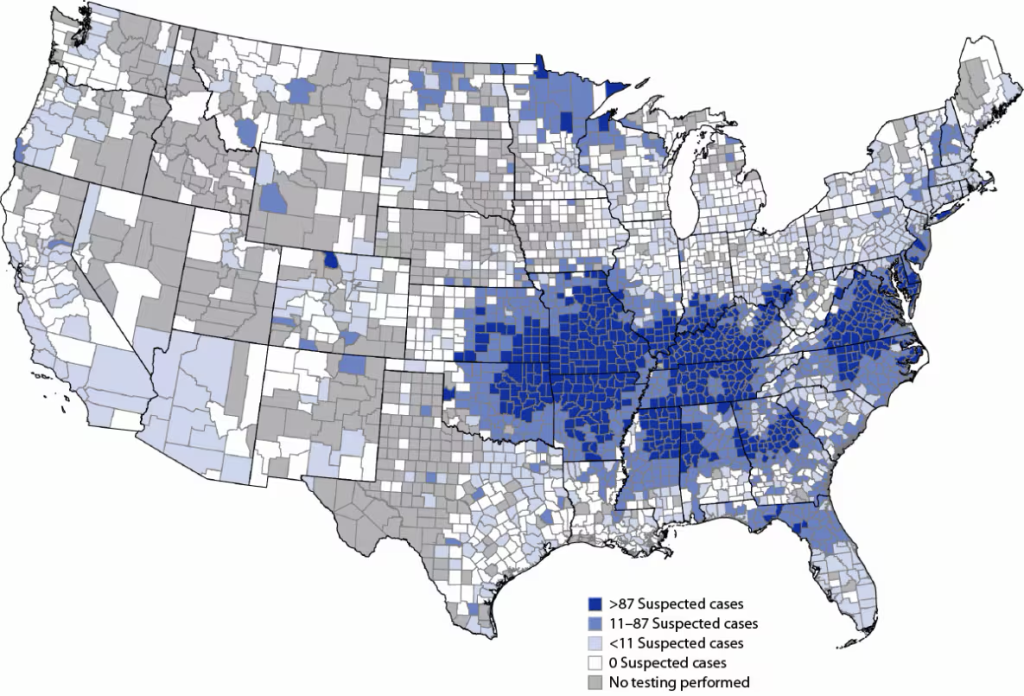
Abbreviations: IgE = immunoglobulin E; IU = international unit; kU = kilounit.
* A suspected case of alpha-gal syndrome was defined as being in a person who had confirmatory laboratory evidence (serum or plasma alpha-gal–specific IgE ≥0.1 IU/mL or ≥0.1 kU/L) with no clinical information available.